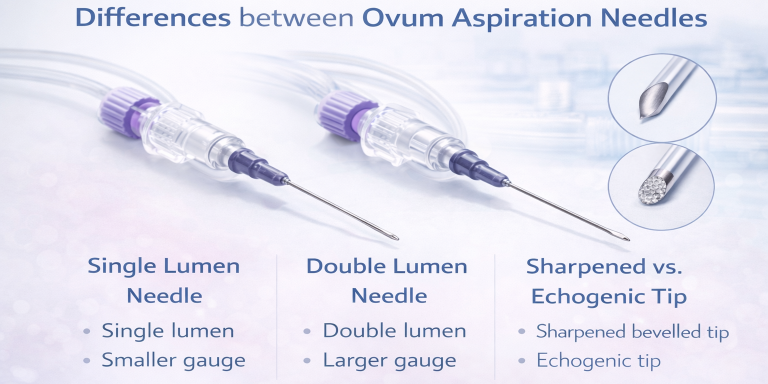
The primary differences between Ovum Aspiration Needles (also known as Oocyte Retrieval or Follicular Aspiration Needles)
usually lie in their design, gauge (thickness), tip configuration, and whether they are single-use or reusable. Here is a breakdown of the key distinctions:
- 1. Needle Gauge (Thickness)
This is the most significant difference.
• 16G and 17G: These are thicker needles. They are generally used for patients with a high number of follicles or when the ovaries are difficult to access. The larger lumen (inner diameter) allows for faster aspiration and reduces the likelihood of the follicle collapsing or the egg getting damaged by suction pressure.
• 18G and 19G: These are thinner needles. They are often preferred for patients with fewer follicles or when the ovaries are very accessible and mobile. Thinner needles may cause less discomfort and trauma to the ovarian tissue, but they require more careful suction control. - 2. Tip Design
• Ultrasound Echogenic Tip: Most modern needles have a textured or etched tip that reflects ultrasound waves, making the needle highly visible on the monitor during the procedure.
• Sharp vs. Blunt:
• Sharp tips penetrate tissue and the ovarian capsule easily.
• Blunt (or rounded) tips are designed to minimize trauma to surrounding blood vessels and organs, though they may require slightly more force to penetrate the ovary. - 3. Single-Use (Disposable) vs. Reusable
• Disposable Needles: These are the standard in modern clinics due to safety regulations. They eliminate the risk of cross-contamination and infection (such as HIV or Hepatitis). They are typically sterile and come pre-packaged.
• Reusable Needles: These are made of high-grade stainless steel and can be autoclaved. While they are cost-effective over time, they require strict sterilization protocols and carry a higher risk of infection if not sterilized perfectly. They may also become dull over time. - 4. Length
• Needles come in various lengths, typically ranging from 350mm (13.7 inches) to 200mm (8 inches).
• The choice depends on the patient’s anatomy and the position of the ovaries. A longer needle might be required for patients with a high body mass index (BMI) or retroverted uterus. - 5. Double Lumen vs. Single Lumen
• Single Lumen: Has one channel for both aspiration and flushing (if needed).
• Double Lumen: Has two channels—one for aspiration and one for flushing follicles with culture media. This is often used in difficult cases to ensure the egg is retrieved from the follicle.
Feature | Option A | Option B |
Gauge | 16G / 17G (Thicker, faster flow) | 18G / 19G (Thinner, less trauma) |
Usage | Single-use (Disposable) | Reusable (Requires sterilization) |
Tip | Echogenic (Visible on ultrasound) | Non-echogenic (Harder to see) |
Lumen | Single Lumen | Double Lumen (Allows flushing) |
The choice of needle depends on the doctor’s preference, the patient’s anatomy, and the specific requirements of the IVF protocol.
Key Factors to Consider When Choosing the “Best” Needle:
• Gauge (Thickness):
The most common sizes are 16G, 17G, and 18G.
• 16G: Larger lumen, faster aspiration, but slightly more discomfort.
• 17G & 18G: Thinner, generally cause less pain and bleeding, but may require slightly higher aspiration pressure.
• Echogenicity:
The needle must be clearly visible on the ultrasound screen to guide the physician accurately. High-quality echogenic markers are crucial.
• Tip Design:
A sharp, beveled tip reduces the force required to puncture the follicle and minimizes ovarian trauma.
• Single vs. Double Lumen: Double lumen needles allow for flushing of the follicle, which can increase retrieval rates in difficult cases, though single lumen is often sufficient for standard cases.